Not medical advice. This article is about telehealth adoption and consumer trends, not personal medical guidance. Always talk to a licensed clinician before starting or changing any medication, and before beginning a new exercise plan if you have health concerns.
Telehealth didn’t fade away after the pandemic “peak.” It shifted into something more permanent: a normal way many people start care, ask follow-up questions, and handle ongoing programs — especially when convenience and speed matter.
That doesn’t mean telehealth is taking over everything. But the overall direction is clear: more providers offer it, more systems build workflows around it, and a lot of patients now expect it as a standard option.
Federal data and health-system surveys show the same story from different angles:
- 95% of HRSA-funded health centers used telehealth to provide primary care in 2024, according to HHS’s Telehealth Trends hub.
- In Medicare fee-for-service, 25% of eligible users had at least one telehealth service in 2024 (flat vs 2023), based on CMS claims analysis.
- Among U.S. adults overall, telemedicine use dropped from 37.0% (2021) to 30.1% (2022) in the National Health Interview Survey — still far above pre-pandemic levels, but a reminder that usage isn’t just straight up and to the right.
So why are telehealth apps still “growing” as a category if some population-level usage has cooled from the peak? Because a lot of growth is happening in specific care pathways (chronic care, follow-ups, convenience-driven programs, behavior health, specialty onboarding) and because health systems have continued building “digital front doors” even after the emergency phase.
McKinsey’s consumer surveys, for example, show telehealth is no longer only a “young person thing”: in 2023, 39% of people under 65 reported using telehealth vs 32% of those 65+, narrowing the age gap compared to 2019.
What’s driving telehealth app adoption right now
1) The “digital front door” is becoming the default
Many health systems now treat virtual care as a first step, not a backup. A Teladoc Health + Becker’s Healthcare annual benchmark survey (hospital/health-system focused) reported that the 2024 study measuring plans for 2025 was the first where 100% of respondents either offered virtual care or expected to by the end of the year.
2) It fits how people actually live
If you’re juggling work, kids, travel, or just don’t want to burn half a day for a short follow-up, telehealth is often “good enough” — especially for routine check-ins and medication management where the clinician mainly needs history, symptoms, and/or labs already on file.
3) Access issues didn’t disappear
Transportation, rural access, and provider shortages are still real constraints. Telehealth doesn’t solve everything, but it can reduce friction in the parts of care that don’t require a hands-on exam.
4) Telehealth isn’t one thing anymore
The public tends to think “video visit.” In reality, a lot of telehealth happens via secure messaging, async intake flows, remote monitoring, and hybrid models.
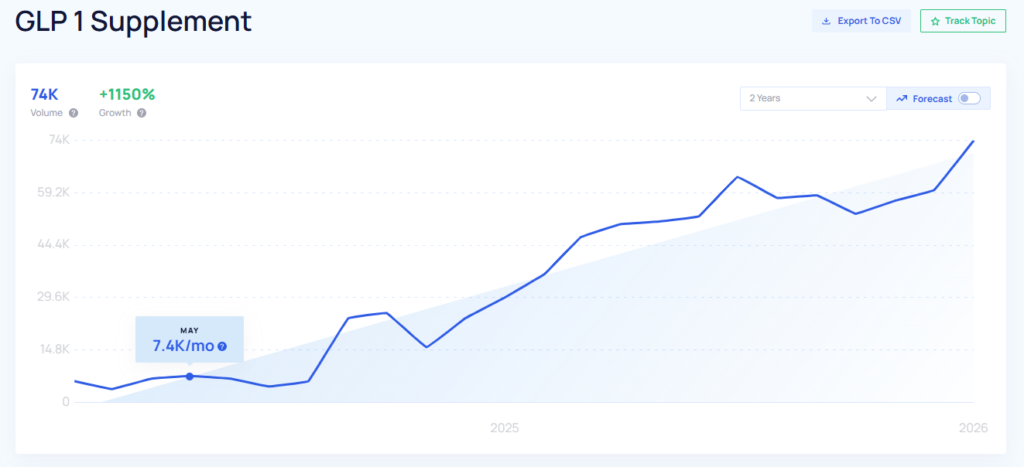
The LevelsRx angle: “1,000%+ YoY growth” (company-reported)
In a recent interview with our editorial team, LevelsRx’s CEO said the company’s new-user growth is “in the order of 1,000%+ year over year.” This figure is company-reported (not independently audited in public datasets), and growth percentages can look especially dramatic when a program is scaling from a smaller base.
Still, the claim lines up with what many telehealth operators have been seeing: when a service hits product-market fit for a specific need — and it removes friction (appointment availability, logistics, ongoing follow-up) — adoption can spike fast.
LevelsRx describes itself as a clinician-guided online weight management platform, with a workflow that begins with intake, moves into provider evaluation, and then continues through follow-ups and support. (And to be clear: this article is not endorsing any provider — it’s highlighting one data point from an operator inside the space.)
Why big telehealth growth claims need context
If you’re reporting responsibly on telehealth, it helps to keep two truths in your head at once:
- Macro usage can plateau (or even dip) while
- Specific niches can explode (because they’re still being built out)
For example, CMS data shows Medicare FFS telehealth usage stabilized at 25% in both 2023 and 2024. That’s not “telehealth is dying.” It’s “telehealth found a baseline level of routine use in Medicare.”
Meanwhile, a company focused on a particular workflow (like onboarding + follow-up care in a high-demand category) can legitimately see triple- or quadruple-digit growth while the overall population percentage barely moves.
What readers should take away (without the hype)
Telehealth apps are becoming more “normal” in U.S. healthcare, but the real story isn’t that everyone is suddenly seeing doctors online every week. It’s that:
- providers and health systems increasingly offer virtual care as a standard modality
- public programs like Medicare have maintained meaningful ongoing telehealth use
- and consumers across age groups continue adopting it for convenience and access
And from the business side, operators like LevelsRx say demand is strong enough to drive dramatic growth — including a 1,000%+ YoY new-user growth figure shared directly by the company’s CEO in our interview

